Professionals were concerned about their patients’ therapies because it is known that long periods of inactivity can worsen symptoms. So, it was important that, given the impossibility of providing therapies at home and in APM centres, those affected by Parkinson’s disease could continue their therapies at home.
In this context, APM started providing physiotherapy, speech therapy, and psychological care, using new technologies, allowing us to maintain contact with patients. Although everything changed very quickly, APM’s response unfolded in stages.
At first, APM used social networks such as Twitter, LinkedIn, and Facebook to share exercise infographics. This enabled patients to follow therapeutic instructions. However, the lack of personal contact sometimes made it difficult to follow the steps laid out in the infographics. Sometimes patients phoned the association to request further explanations, sharing their difficulties in carrying out some of the exercises. Dealing with this aspect over the phone was very difficult for APM therapists.
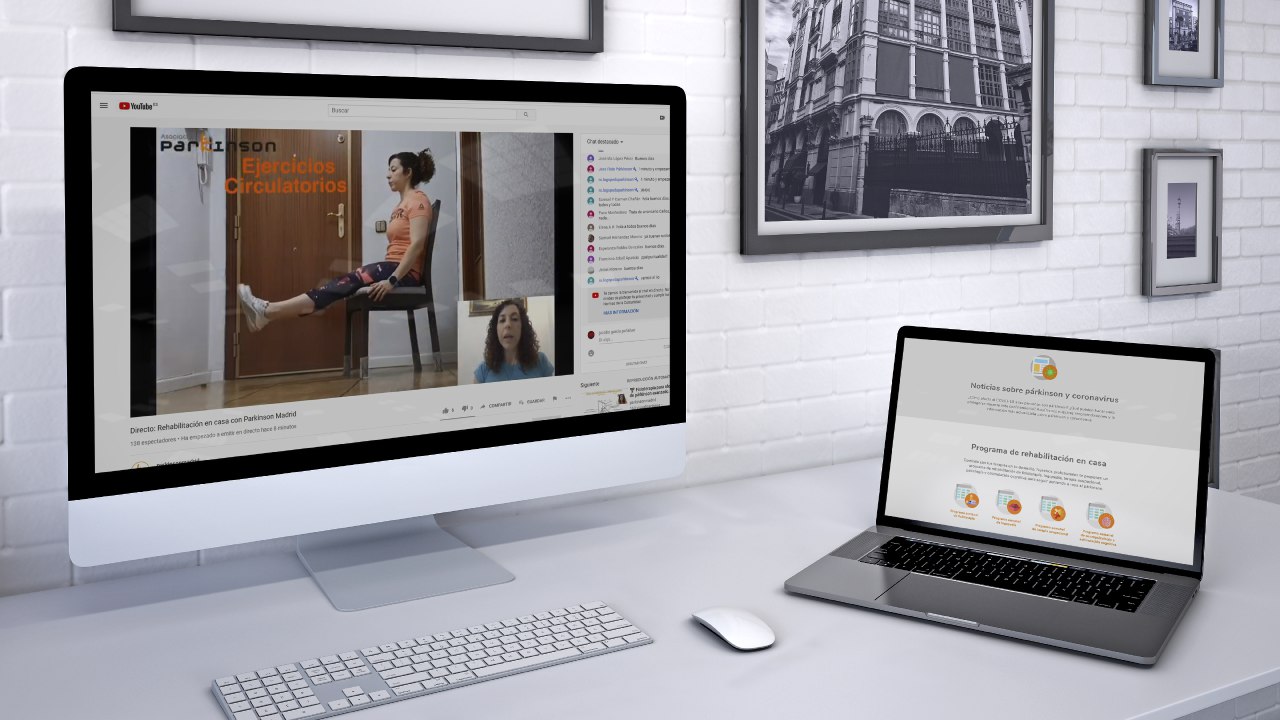
The next step involved streaming the therapy sessions. The videos with the exercises performed by the therapist were previously recorded. Space and the home conditions were taken into account. The interaction in the YouTube chat was very positive, both between the patients and with the therapists, an aspect that was useful in improving the sessions.
The last step was to develop one-on-one tele-rehabilitation, which allowed patients to choose different rehabilitation sessions and have direct contact with their therapists.
APM therapists Jessica Jiménez Cruz and Rocío Martín Picazo, who were involved in this entire process, shared their experiences, pointing out the most positive aspects and the aspects that need to be improved.
Among the aspects that need to be improved, they both point out that there is still a technological gap in regard to older people’s digital skills. Older patients often turned to their relatives, grandchildren, and caregivers to overcome this difficulty and many learned from them. The gap remains, however.
From the technical point of view there was also an internal learning process, the first videos are of less quality compared to later ones where lighting or positioning were considered. Another issue that arose concerned the lack of interoperability between some of the devices, software, and video formats.
One of the positive aspects of tele-rehabilitation that Jessica Jiménez pointed out, has been that it allows therapists to personalise the sessions; that is, it allows people affected by Parkinson’s disease and their families to use this tele-space with their therapist to fit their specific needs. In addition, this experience has provided a new working model for professionals who until now were not usually considered for telework.
For Asociación Parkinson Madrid, there is no doubt that new technologies are the future and that more and more will be introduced in the field of health. Our next steps will include improving tele-rehabilitation and making it more accessible for a greater number of older people by helping them bridge the technological gap and adapt to a new reality.