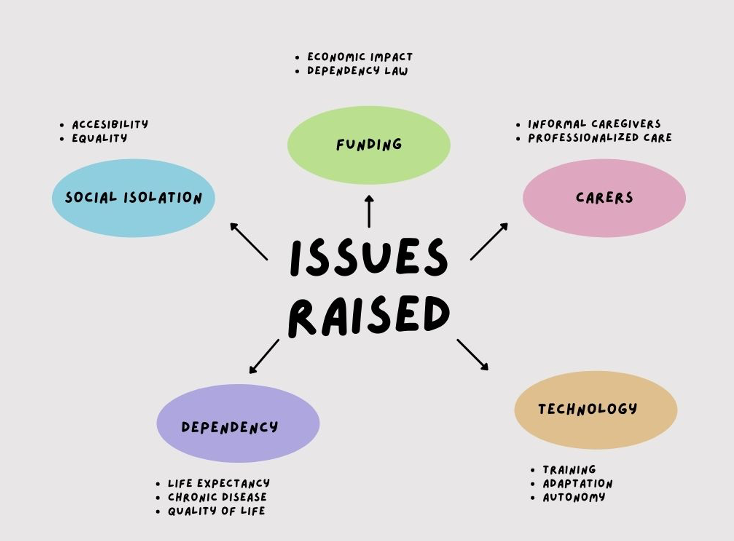
To help elderly patients preserve their autonomy and live at home longer, some receive treatment at home. In this context, it is possible that they may experience a critical situation that will require further medical assistance.
Continue readingUnderstanding the impact of COVID-19 on the quality of life of chronic patients
The arrival of the Covid-19 pandemic has had a significant impact on the lives of the entire world population, but if we also consider the impact on people affected by different chronic diseases, such as Alzheimer’s, Parkinson’s disease (PD), or cardiovascular pathologies, the scope is even greater.
Continue readingData-sharing for precision medicine & the well-being of people with dementia
In precision medicine, the focus is on identifying which approaches will be effective for patients based on genetic, environmental, and lifestyle factors.
Continue readingModern eHealth applications
The adoption of a well-designed eHealth application in everyday health practice can provide holistic solutions to extend the autonomy of patients while improving their Quality of Life (QoL).
Continue readingTeNDER’s QoL Assessment methodology to be presented at conference in Corfu
We will also present a description of the QoL assessment questionnaires for participants (patients, caregivers, professionals) elaborated by the TeNDER consortium.
Continue readingWhat is open source?
The first software built was proprietary, which means that access to the source code was restricted and only creators could make changes to it. As time went by the term open source was born.
Continue readingFragmented eHealth regulation in the EU
One of the goals of the European Commission has been to build a robust health union, including by addressing eHealth regulations.
Continue readingThe TeNDER home tracking system
One of the main objectives of the TeNDER project is to improve the Quality of Life of patients. This means, among other things, to increase safety perceptions, not only in patients but in family members and caregivers.
Continue readingDigital health and social impact
Digital technologies are essential components of sustainable health systems and universal health coverage. To realise their potential, digital health initiatives must centre around the wider health needs of the population and be integrated into the digital health ecosystem.
Continue readingArtificial Intelligence and Health
The mention of artificial intelligence (AI) often conjures the figures of industry consultants and tech moguls overhyping it, dystopic images of superintelligences superseding ours, or the very real headlines of issues arising during the early adoption of certain systems, e.g., face recognition.
Continue reading